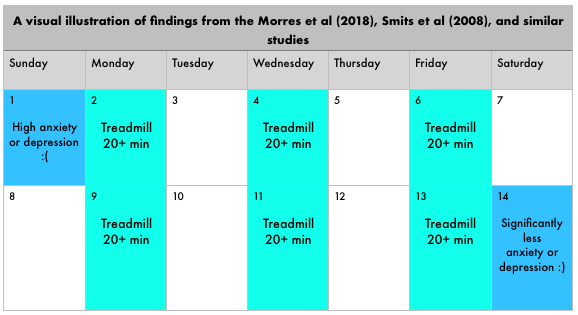
"If Exercise were a Pill, everyone would be taking it."Gif credit: Jamie Farrell My husband and I brought our son on his first wilderness canoeing trip this week (he fell asleep -- until I accidentally splashed him!) I am instructing a few day kayaking programs this summer, as well as updating the MHWFA curriculum for the fall, and reflecting how meaningful it is to make time for movement in supporting good mental health. As a seasonal kayak guide for 15 years, working physically every day outdoors did a world of good for my mood and anxiety levels as well (October was always a different story!). So, this newsletter is dedicated to the mental health benefits of exercise. There is no shortage of scientific research on the mental health benefits of regular exercise. Regular aerobic exercise is one of the most effective treatments (with few side effects) available for mild to moderate depression, and it also has been found to improve the effectiveness of other interventions such as antidepressant medications and cognitive behaviour therapy. And not just mood disorders: exercise has been found effective for treating those with post-traumatic stress disorder and schizophrenia as well as anxiety disorders. In a particularly memorable study, assigning individuals to a routine of just three 20-minute treadmill sessions per week for two weeks was sufficient to result in clinically decreased levels of anxiety. Many of our MHWFA students are folks who work outside or physically in some way: treeplanters, SAR volunteers, outdoor educators, traditional medicine gatherers. For some people, 20 minutes of exercise three times per week feels like a lot! At the same time, remote area living/working/playing frequently involves more than 20 minutes per day of physical activity. So, two things for our students:
0 Comments
I was delighted when I found this book during my Master's studies, as I recognized the names of the authors from many of the scientific articles I was compiling at the time for my final thesis project.
Smits and Otto, both PhDs, do a great job offering an incredible amount of clinical knowledge in an easily accessible, helpful format. Reading this book feels much like a conversation with a personal coach, walking you through some great research on the science of exercise and mood as well as a plan for setting up and maintaining the motivation for your own exercise routine. There are short, fill-in workbook style exercises for you to complete about your own exercise journey, and snippets and anecdotes about "regular Joes" and professional athletes -- many of whom struggle with mental health and motivation, too. They explore the science of motivation, warn you about excuses that come up and problem-solve ahead of time for how to avoid them: When you are down, blue, or sad, it is sorely tempting to skip a workout. But, as you hear yourself say, "I don't feel like it," remember that this is the very time at which exercise is most likely to help. Choosing not to exercise because you are feeling down is like choosing not to take an aspirin because you have a headache. (91) MHWFA students will recognize a combination of psychoeducation, cognitive behaviour, and "solution-focused conversation" techniques in a book that is nicely practical as well as theoretical. And for those of us who work seasonally, this may be just the right tool to help you develop your awareness for how the changing seasons can affect your own mental health, and put together a plan for the coming year. Note: I don't use affiliate links, and the Recommended Resources section is not sponsored. I (Daye) only tell you about books I have actualy found useful professionally or personally. Confession time: I (Daye) have not one but SIX copies of this book (and its sister books, How to Talk So Teens Will Listen & Listen So Teens Will Talk, and How to Talk So Kids Can Learn) on my bookshelf. As I say in class: whenever I find a copy at a thrift store, I buy it, because I love to give them away.
How to Talk was originally published in 1980, by Adele Faber and Elaine Mazlish. It's been revised and sold millions of copies since. I remember seeing it on my Mom's nightstand when I was a kid. "That's dumb," I thought at the time; "she'll never get that to work on me." (In retrospect, seven-year-old-me was wrong; it wasn't, and she did). Decades later, as an adult, I rediscovered the book when working as an outdoor educator at Strathcona Park Lodge. It opens with one of my favourite lines: "I was a great parent before I had kids." (Now Mom to a 4-month-old; can confirm). Filled with cartoons, anecdotes, and humour, How to Talk is an effective and empathetic primer on communicating with humans of any age. At Strathcona, I realized it was changing the way I talked to the schoolkids I worked with, but also how I was talking to my co-workers and friends. I eventually started running workshops based on How To Talk for other outdoor educators there. I can confidently say this book was the beginning of a path that saw me going back to school to become a counsellor. In honour of Mother's Day, I'm highlighting How to Talk as our resource of the month. Look for it at a thrift store near you -- or try here. Tara is a veteran wilderness guide and clinical counsellor working out of Ucluelet, B.C., and specializing in grief, loss, and nature-based therapy. This workshop is an opportunity to explore ways we can incorporate nature-based healing practices into any outdoor activity. Accessing nature as a healing partner allows for creative, spontaneous and unique self-generated insights and thus deepens the conversations around the healing journey. Nature, whether it be in a vast wilderness or a city park, is accessible to every person, and building nature-connection remains available to us as a resource throughout the lifespan. This workshop shares specific exercises and activities that can be used with clients and for ourselves personally or professionally. Video coming soon! 3/31/2022 Guest speaker Jeremy Addleman: Trauma and Healing from a somatic psychotherapy perspectiveRead NowMental Health Wilderness First Aid Guest Speaker Jeremy Addleman, C.C.C., March 30, 2022 RESILIENCE & RECOVERY: THE POWER OF NATURE TO AID IN HEALING TRAUMA FROM A SOMATIC PSYCHOTHERAPY PERSPECTIVE Jeremy is a trauma therapist at Point the Way Counselling in Victoria, B.C., specializing in somatic psychotherapy, looking at trauma and healing through the body and nervous system. "In this workshop I provide information on how to use principles of somatic psychotherapy, in combination with the natural world, to build resilience and aid trauma recovery while out on the land. Together, we will examine brief ideas of the nervous system and how using mindfulness and somatic psychotherapy concepts and practices in nature can help when dealing with stress and trauma in other situations in life, as well as in the field." "[During my MHWFA course I kept thinking, 'When am I going to use this? It's all great, but I have no idea when I'm going to use it.' Well, since the fire, I have been going back to that course over and over and over again. There's things that we're going to talk about today -- the Lizard Brain and the Wizard Brain, I have probably explained that 50 times [to others affected by the fire] since January." with The Marshall Fire tore through the Colorado communities of Louisville, Superior, and Boulder County, starting just before New Year's Eve 2021-2022. Colorado resident Cathryn Marsh, one of our MHWFA alumni who evacuated with her family during the fire, contacted MHWFA to ask if we could support the community by offering a workshop on trauma healing for those affected by the fires. Here's an excerpt from Cathryn's introduction for our presentation: Cathryn: "It was about June or July 2021 that I was trying to look for how to tie together my wilderness medical training, and this personal trauma work that I had started. So, I started to look for courses that bridged the gap. And strangely enough, I came across Mental Health Wilderness First Aid, and it happened to be in Canada. Because of the pandemic, they had gone online ... [The course] was 4 weeks in November, two and a half hours every week, and I learned all this stuff and I kept thinking, 'When am I going to use this? It's all great, but I have no idea when I'm going to use it.' Well, since the fire, I have been going back to that course over and over and over again. There's things that we're going to talk about today -- the Lizard Brain and the Wizard Brain, I have probably explained that 50 times [to others affected by the fire] since January. How to bring yourself back from that trauma swirl and get grounded, I do that probably 4 or 5 times a day. And then how to 'hold space' for other people, and active listening ... there are really some techniques [we learned] for how to effectively hold space for other people." Daye's presentation covered four topics:
In particular, we talked about common characteristics of activities that promote healing and resilience to the part of the brain affected by trauma: Daye: "This is something that we know about the part of the brain called the limbic system [which is affected by trauma]. The limbic system responds to rhythm, it responds to repetition, and it responds to relationship. So, the part of the brain that initiates the fight/flight/freeze response, especially if it's going through "sticky fight/flight/freeze" [trauma], it will help to regulate this part of the brain to do activities that have rhythm, that have repetition, and especially activities that also have relationship. So, what are some examples? ... there are some activities that we naturally do like going for a walk. We can also return to the breath ... sometimes when we experience stress or trauma, it's almost as if we are holding our breath for a long time. We might feel like we haven't taken a deep breath all day -- or for months. Other things that are naturally healing and regulating for the lizard brain -- things that are rhythmic, repetitive, and relational -- going skiing, going skateboarding; skateboarding's really good for young people; you can see that through a resilience-based lens, it's something that's naturally healing for their brains." Together, we talked about and practiced several different short activities that hit those "rhythmic, repetitive, relational" goals: swimming, paddleboarding, biking, music, prayer, reciting simple math problems. We threw our socks around in sync -- no small task over Zoom! -- and tried out "Tapping" together, which is a simple, evidence-based strategy for regulating the nervous system that can even be fun. Daye additionally covered the topic of supporting children who have experienced of trauma, including the importance of play for the developing and healing child's brain, and Cathryn Marsh provided a multitude of local area resources. A comprehensive document including all presentation notes and resources for those affected by the Marshall Fire is posted directly below.
Joelle is a clinical counsellor and author. She works in private practice online in British Columbia, specializing in communication, trauma, and anxiety. In November 2021 she published The Conversation Guide. On February 13th (in honour of Valentine's Day and Family Day), Joelle joined us for an interactive presentation about boundaries - what they are, why we need them, how to have conversations about them, and why we avoid these conversations! We also discussed difficult conversations in general, how to structure them, and why it's important to have them.  As a seasonal guide, I (Daye) averaged 100-140 days in the field, from surf beaches to old growth trails. I often told people, "I get to wake up each morning thinking, 'There's nowhere else in the world I would rather be today' - not everybody has that." Guiding and the outdoors got me through a lot in life, and helped strengthen me in to the person I am. At the same time, as this all-too-short article from Outside Magazine touches on, the changing of the seasons each November brought with it a predictable shift in spirit. My work was 3 seasons: my love affair with water in its liquid form only. Each winter I felt like I was floundering, drowning even, as I struggled to patch together income, housing, and relationships, knowing that the following spring would bring further change. I predictably spiralled further in to self-doubt, mood disruption, and shame each successive fall. Although I loved the seasonal work, it was this annual instability that played a primary motivation for me to pursue a Master's degree and a career change to become a clinical counsellor. Now, I integrate outdoor and guiding work in a different way, with mental health as a personal and professional focus -- but it's taken a lot to get here. Read the Outside Magazine article at: https://www.outsideonline.com/health/wellness/seasonal-guide-mental-health-stress/ Join Daye for a snowy winter walk as she introduces a few mental health practices in nature. How many of these techniques do you remember from your MHWFA Basic class? Covered in this video:
2021 was a wonderful year of growth! We worked with:
Why are people often naturally drawn to outdoor activities like skateboarding, surfing, treeplanting, and paddling, that offer rhythmic movement and relationship-building in nature?
Sarah Hagar, M.Ed., R.C.C., is a former veteran treeplanter and Registered Clinical Counsellor with a keen interest in healing and preventing trauma for children, youth and families. With training in neuroscience and the belief that we are drawn to what heals us, Sarah offers a conversation that explores why we function the way we do, the neurobiology of natural healing activities outdoors, and empowers you towards doing more of what makes you feel whole.
A note with resources from Sarah
Hi there, Some links to share: The Neurosequential Model of Therapeutics: Home | NMnetwork Child Trauma Academy: HOME | ChildTrauma Academy Bal a vis x: HOME Shawn Ginwright, PHD, on Healing-Centred Engagement: The Future of Healing: Shifting From Trauma Informed Care to Healing CenTERED ENGAGEMENT Marie Jose Dhaese: Centre For Expressive Therapy - Centre for Expressive Therapy Centre For Expressive Therapy - Centre for Expressive Therapy Interested in learning more about Rites of Passage in Nature? School of Lost Borders – Teaching the Rites of Passage Since 1981. School of Lost Borders – Teaching the Rites of Passage Since 1981. Thanks for the opportunity to share, Sarah Highlighted clip (6:36) Full video available to watch at the bottom of this page. Michael McCarthy, a Yuułuʔiłʔatḥ and Hesquiaht First Nations member, is a clinical counsellor and regional coordinator at Nuu-chah-nulth Tribal Council (NTC). An accomplished public speaker, Michael thrives in the intersection of western psychotherapy and traditional cultural healing teachings -- "What my Granny taught me". As an NTC coordinator, Michael has frequently guided Daye Cooper Hagel and other mental health clinicians in weaving traditional and western mental health teachings -- "walking in two worlds". In this spirit and time of Truth and Reconciliation, what does each mode of healing have to offer the other? "All pre-industrialized communities, regardless of where you’re from, had practices that kept you healthy. We just need to remember those practices. So for us, being Nuuchahnulth, being on the west coast, going in to the water, cold water, immersing ourselves, is a way of our healing practice. ... And for those that go and use cryotherapy or cold water therapy, the first time you dunk under, full immersion under the water, you come out and you [gasp], and you have this convulsion, this involuntary vocalization, and my teachers would say, that [gasping] is me letting go of the things I needed to let go of. And this is the interesting part: our brain chemically and mentally can’t make the distinction between that [gasping] and a big grief cry, and so we naturally feel much better when we’re in the process of doing this … So, when we do that ritual of bathing where I’m from, it’s a way to truly maintain that good mental health." Michael's full talk (1:18:36)
Your health care decisions are personal. Medical and therapeutic ethics are fundamentally important. The B.C. provincial government has announced a mandate that as of September 13, 2021, proof of having received one or more experimental COVID-19 injections will be required as a condition of full participation in public life. Mental Health Wilderness First Aid opposes this profound violation of Canadians' constitutional rights and of medical and therapeutic ethics. We respect the legal and moral rights of all Canadians to privacy and fundamental liberties. We will not be requiring health passes of our staff, contractors, or students as a condition of participating in our programs.
Health passes, or vaccine passports, create a system of legal coercion and medical apartheid that violates both the Canadian Charter of Rights & Freedoms and the Nuremberg Code as well as basic ethical guidelines. It is wrong to coerce someone to undertake a medical procedure. Our duties are to our professional ethics, our conscience, and our civilization, not to an unconstitutional government mandate. We will not help the government violate the Charter nor contribute to the downfall of Canada as a free and just society.  What you can do
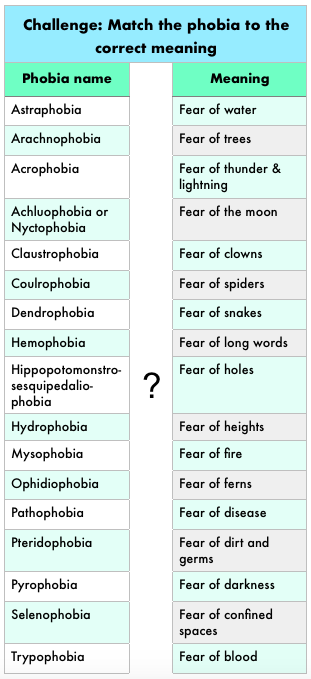
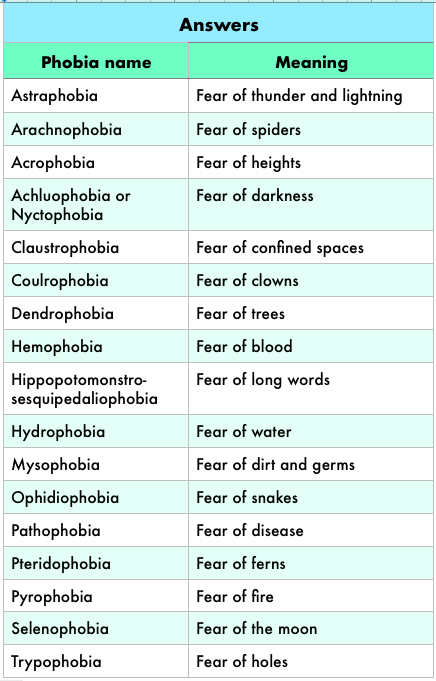
Vaxxed & Unvaxxed Against the Pass “S-s-s-SNAAAAKE!!” The terrified cry came to me from across the campsite where, on the Juan de Fuca trail, I had been guiding a family hiking trip for the past three days. Adrenaline surged through my body and my pulse skyrocketed in response to the emotion in the scream, which turned quickly in to a frantic, high-pitched sob. Before our expedition began, Gabrielle, a high-functioning mom and legal professional from Vancouver, had indicated a strong fear of snakes on her medical form. “I know they’re not poisonous out here,” she wrote. “I can’t help it. If you see a snake, please don’t tell me.” Now, one had suddenly appeared close to her. My muscles tensed as my brain prepared my body to run to her aid. Specific phobias are not uncommon, either in the wilderness or the city. An estimated ten percent of the adult population (and sixteen percent of youth) experiences a strong fear or avoidance reaction to a specific thing or situation that is significantly out of proportion to the actual risk posed. Common phobias include heights, snakes, spiders, elevators, confined spaces, germs, flying, or the dark. Less common phobias I have seen clinically include fish and “small soft things, like rabbits”. However, the object of a phobia may be almost anything. A table below, borrowed from the MHWFA course book, lists 17 different phobia examples which you can try matching up to their correct meanings (answers at the end of the article).
Supporting a Person With Specific Phobia in the Wilderness Take a Deep Breath If you forget everything else, take a deep breath and settle your own nervous system. While I immediately tensed up at Gabrielle’s reaction and wanted to run to her, I tapped in to a thankfully ingrained habit of taking a deep breath, and (heart still pounding) walking to her side. Being around someone who is experiencing phobic response can activate your own fight / flight / freeze system. On the contrary, you providing a calm, nonanxious presence activates the other person’s mirror neurons and naturally will help them to regulate their own emotional responses in a healthy way. Awareness How grateful I was to have had a heads up about Gabrielle’s phobia from her medical form before our expedition began! Although most registration forms ask only about physical health concerns, it is equally invaluable to attune to mental health issues that may arise in the field. Consider incorporating questions from the MHWFA pre-trip mental health form (a free resource available on our website) in to the registration forms for your own organization. Intervention Strategies Plan ahead: when a phobic stimulus is encountered in the field, what strategies will help manage it in the moment? The person may already have their own ideas and strategies established, which you can build on. Diaphragmatic breathing, mindfulness, and tapping are three of my favourite and most effective interventions. When you encounter a phobic stimulus, immediately tune in to and name out loud some of the other simple things you can see, hear, feel, smell, and/or taste around you. Or, try pairing deep “belly breathing” with a gentle, consistent tap on the collarbone, eyebrow, or anywhere else that feels grounding. We can also gently identify and challenge unhealthy, unrealistic cognitions that accompany phobias. Someone with a specific fear of bridges may experience an intrusive thought that “the bridge will collapse as I cross it.” Assuming that the bridge really is solid, of course, a healthy, realistic alternative thought might become a simple self-reminder to repeat: “I am grateful for the strength of this bridge and the skill and care of those who constructed it.” All of these intervention strategies can be incorporated in to a safety plan, which is another free resource available on our website for supporters as well as clients.
Be Aware of Flooding “No thanks; I’m definitely not going to look at a picture of a snake if I don’t have to,” Gabrielle might have said. Would it have been helpful for me to insist? Baby Step Ladders do include risk and must be used cautiously. Flooding may occur if someone is exposed, even voluntarily, to too much of a stimulus too quickly, and the result can be an exacerbated phobic response going forward. Not helpful! If you are considering a Baby Step Ladder, it is wise to both 1) follow the motivation of the client in whether to do so, and 2) have additional support or training in this area (e.g. a self-paced workbook like the Bourne (2015) resource cited below, or training offered by a MHWFA course). Connecting to Resources In the field, we’re doing first aid. Help this person additionally connect to a resource that can support them in ways that they choose in the medium-to-long-term. Some clinicians excel in particular areas; one therapist I saw in Victoria specializes in phobic responses, calling himself the “Fear Doctor”! Other supportive resource options may include a mental health line, physician, counsellor or perhaps an attuned spiritual leader in their community.
Daye and the MHWFA program have been featured in the November 2020 issue of Outside Magazine! The article illustrates the importance of preparing for psychological incidents in wilderness areas, and notes that we are now offering MHWFA classes online (next cohort starts January 6th).
Read the article here. In My Grandmother is Always With Me (one of the books we talk about during the MHWFA Standard course), Addison tells us about the wonderful relationship she has with her Grandmother, who died many years before Addison was born. Our puppets and we discuss some of the people we love most in our lives who have died, and how we continue to remember, share practices, and nurture loving, ongoing relationships with them throughout time. Collin and I had a wonderful time filming this video around Ucluelet. Qwaićiik and Sičpax figure out what self-care during lockdown really means! Continuation of our short series on basic MHWFA skills - conducting feelings check-ins with our loved ones, especially during quarantine situations.
Chims the bear and his family have to stay in their cave. We share some techniques like tapping from our MHWFA class that can help at times when we feel stressed and anxious. |
Details
AuthorDaye Cooper Hagel is a clinical counsellor, veteran wilderness guide, and director of the Mental Health Wilderness First Aid program on the west coast of British Columbia, Canada. Read more about her and the MHWFA on the About Us page! Archives
July 2022
Categories |
|||||||||||||||
About Us |
Courses & Events |
|
|
We do not require personal medical information from our students, volunteers,
staff, or contractors as a condition of providing services. |




















 RSS Feed
RSS Feed
